In keeping up with my out-of-order crazy tire swinging, here are some pictures and reflections from my first chemo treatment on May 8th.
Wow, has the time swung by!
– – – – – – – – – –
10:00 AM: Arrive at outpatient infusion center.
Only two days before my first infusion, I had my port placement surgery. Obviously my chest still felt incredibly bruised and sore from having been cut open and a small foreign object crammed inside it.
I had not yet been able to get my prescription for lidocaine cream, which numbs the skin before a nurse jabs through it and the "soft top" (high grade medical plastic) septum with a needle to access the port.
Add to my predicament a sharp fear of needles, and you've got a recipe for a hurricane of tears, which I did my best to hold back.
My nurse for the day, Cheri was amazing. She listened to my concerns and talked me through the procedure, per my request. As I braced myself for super intense pain— squeezing Mom's hand, closing eyes, tissue ready, big deep breaths, big deep breaths—Cheri accessed the port faster than a dart hitting a bullseye.
Whoa. No tears at all. In fact, I distinctly remember thinking, "That was easier than getting a navel piercing."
(Note: I have to give praise to all of the nurses at the infusion center. Cheri, Terri, Mary, and Jayne are exceptionally skilled at accessing those ports with precision and speed, which leads to minimal discomfort even when I haven't used the lidocaine cream.)
With the drama of needles and port access out of the way, my first infusion continued.
Then, chemo-ification time came! Usually I receive the drugs out of ABVD order. It's more like AVDB or AVBD. The order doesn't matter, as long as it's the correct drug and the correct dosage.
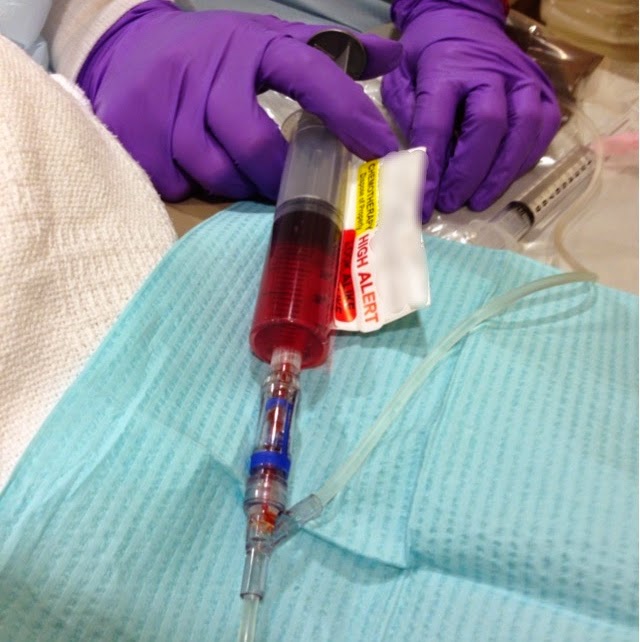
Adriamycin and Vinblastine come in syringes and the nurses "push" each drug in small amounts into my IV. Bleomycin and Dacarbazine hang from the IV pole and are pumped through automatically.
Total chemo time:
Adriamycin: 10 minutes
Vinblastine: 5 minutes
Bleomycin: 30 minutes
Dacarbazine: 60 minutes
 |
| Nurse Cheri and the four chemicals she's about to infuse me with. |
You will note a lack of costume. The advice I received was to "dress comfortably," and dress comfortably I did. The idea to dress in costume originated sometime near the end of my first treatment.
 |
| Almost done for the day! (Oh my goodness! I still had hair back then!) |
2:00 PM: First infusion DONE!
I was surprised I felt as good as I did when I walked out of the infusion center. Mom and I went grocery shopping to pick up some grub for the weekend.
Afterwards, I celebrated my first successful chemo infusion by dressing up and nibbling on a piece of pie. Because everything is better with pie. And steampunk gear.
My Facebook friends might be familiar with this lovely photograph:
It's all smiles and silliness for a little while...
By 4:00 PM the chemo caught up with me and my body felt as if it had gone through a blender.
Yuck.
Just…yuck.
Yet I still tried to attend a small family gathering to celebrate my brother-in-law's birthday. This was the result:
|
|
I've used this pic before, but it captures the distress of chemo day.
|
My mom and I left the party early, and I sat in my shower for a solid thirty minutes letting warm water soothe me. I had an evening snack of fruits and veggies, and my body felt better. Lots of rest over the weekend also helped.
– – – – – – – – – –
So, that was my first chemo experience. Of course, over the next two weeks there were a lot of side effects and gross days and ickiness that I'm glad are in the past.
I've adjusted over time and basically become a pro at it now.
Most chemo days have followed a similar pattern: wake up, apply lidocaine cream, rest/nap while getting infused, endure nausea, return home, sleep off the side effects the rest of the day and most of the weekend. Take pain relievers and warm showers as needed.
Also über important: Take anti-nausea meds on time.
It's weird to think I'm almost done, and also super relieving. The first treatment is rough because neither you nor your body knows what to expect, and it's only the beginning. Looking back is kind of empowering because Hell yeah, I did it!
Well, I've almost done it.
Only one more to go!